In the NICU, time is often our most precious resource. Few conditions prove this more than Hypoxic Ischemic Encephalopathy (HIE). When a newborn is deprived of oxygen around the time of birth, the brain injury isn’t a single, static event. Instead, it’s an evolving process that unfolds over hours and days.
This is why neonatologists are so hyper-focused on the first six hours of life. In a recent teaching session, Prof. NB Mathur broke down the phases of HIE in a way that moves past the textbooks and into real-world clinical practice. Once you see the timeline, the “why” behind our treatments becomes crystal clear.
Watch Session: Phases of Hypoxic Ischemic Encephalopathy (HIE): Pathophysiology & Clinical Window | Prof. NB Mathur
1. Primary Energy Failure: The Initial Hit
This phase happens within minutes of the hypoxic event. When oxygen and glucose levels plummet, the brain’s “power plants” fail.
Without enough ATP (energy), the cellular pumps that maintain balance stop working. Sodium and calcium flood into the cells, causing them to swell. The chemical chain reaction looks something like this:
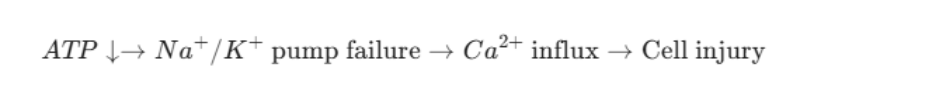
As this is happening, several fires start at once: lactate levels rise, glutamate is released, and oxidative stress begins. While some neurons die immediately, many others are “stunned”—damaged but still salvageable if we act fast.
2. The Latent Phase: Our “Golden Window”
After the initial crisis, there is often a deceptive period of calm called the Latent Phase, usually lasting between 1 to 6 hours.
During this time:
- Resuscitation has stabilized the baby’s circulation.
- Oxygen supply has partially returned.
- ATP production temporarily ticks back up.
Clinically, this phase can be a “trap.” The baby might look relatively stable, leading to a false sense of security. But under the surface, the injury is quietly simmering. Calcium overload and mitochondrial dysfunction are still active.
This is the most critical window in HIE management. Therapeutic hypothermia (cooling) is most effective during these first six hours. For residents, remembering this window is the difference between reactive and proactive care.
3. Secondary Energy Failure: The Second Wave
Starting around the 6-hour mark and lasting up to 48 hours, the Secondary Phase (or reperfusion injury) begins.
It sounds counterintuitive—why does the brain get worse once blood flow returns?
Even with oxygen available, the damaged mitochondria can’t use it. Inflammatory “alarms” (cytokines like TNF-alpha and IL-6) go off, further damaging neurons and the brain’s white matter. This is when the most significant, permanent neuronal loss often occurs.
4. The Tertiary Phase: The Long Road to Recovery
The Tertiary Phase begins weeks after the initial event and can last for months. This is a complex period where the brain is simultaneously dealing with chronic inflammation and trying to repair itself.
While the damage may continue, the brain also shows incredible plasticity. Through neurogenesis and remodeling, the brain attempts to rewire. This is why long-term developmental follow-up is non-negotiable; we aren’t just treating a baby in the NICU, we are managing their potential for the rest of their life.
Why This Matters for Residents?
HIE can feel like an overwhelming mountain of pathways and terminology. But when you look at it as a timeline, it becomes a clinical map.
You start to see why the “Golden Six Hours” isn’t just a catchphrase—it’s the only time we have to truly change the trajectory of the injury. When you understand these phases, HIE stops being a topic you memorize for rounds and starts being something you can actually visualize at the bedside.
Want to get deeper into clinical pediatrics?
If you found this helpful, the Conceptual Pediatrics App offers many more high-yield sessions designed specifically for residents. From NICU protocols to emergency cases, we focus on simplifying the complex so you can focus on your patients.










